Nirvana
My Role
User Research
System Design
Prototyping
Application Design
Tools
Figma
Illustrator
Photoshop
InDesign
Premiere Pro
Team
Solo Project
Duration
4 Months
Background
In India, a silent pandemic of Type 2 Diabetes impacts millions, disrupting physical health, daily routines, mental well-being, and financial stability. The rising incidence of early-onset Type 2 diabetes poses challenges to public health, strains the healthcare system, and imposes economic burdens.
0
Million
of Indian population above the age of 18 years are suffering from diabetes.
0
Million
are prediabetics (at a higher risk of developing diabetes in near future).
0
Percentage
of people are unaware of their diabetic status.
How might we provide early support for middle-aged Type 2 diabetic and prediabetic patients to address their holistic needs throughout their period of uncertainty and denial for better management of their condition to delay the onset of diabetes?
Research
Autoethnography
Type 2 diabetic and pre-diabetic individuals photograph their daily meals to understand their dietary habits, portion sizes, meal timings, and nutritional awareness.
- Lack of basic nutritional knowledge highlights the need for improved education.
- Irregular meal schedules and excessive carbohydrate intake emphasize the importance of structured planning for effective diabetes management.
- Cultural influences, emotional eating, and food accessibility are significant factors in diabetic patients’ dietary choices.
Clinical Trial Observation
Participated in the home-based sample and data collection for diabetes research at the Madras Diabetes Research Institute,involving 16 participants of varied ages.
- High rates of co-existing conditions like hypertension and high cholesterol were observed in Chennai’s Type 2 diabetes population.
- Family history of diabetes increases risk, hinting at genetic and environmental influences.
- Inconsistent adherence to treatment plans and medications is a common challenge.
Qualitative Interview
After conducting secondary research, qualitative interviews were conducted to address critical aspects of diabetes care, focusing on understanding challenges in individuals with type 2 diabetes.
Quotes from Doctors
“When diabetes is treated early and the body’s sugar levels are effectively managed, the body retains this memory. This is called metabolic memory. As a result, even if sugar levels fluctuate in the future, it will not lead to complications.”
- Dr.Jagadish, Diabetologist, Mohan’s Diabetes Specialities Centre
“The initial 5 to 10 years are crucial period for maintaining blood sugar under control. Subsequent phases of diabetes become more manageable by controlling complications, known as legacy effects.”
- Dr.Thangamani, Nutritionist, Mohan’s Diabetes Specialities Centre
“Patients often struggle to accept their diabetes diagnosis and the need for lifelong medication. This can lead to anger and depression.”
– Dr. Vidyalatha Ashok, Psychologist, Mohan’s Diabetes Specialities Centre
Quotes from Middle-Aged Diabetic Patients
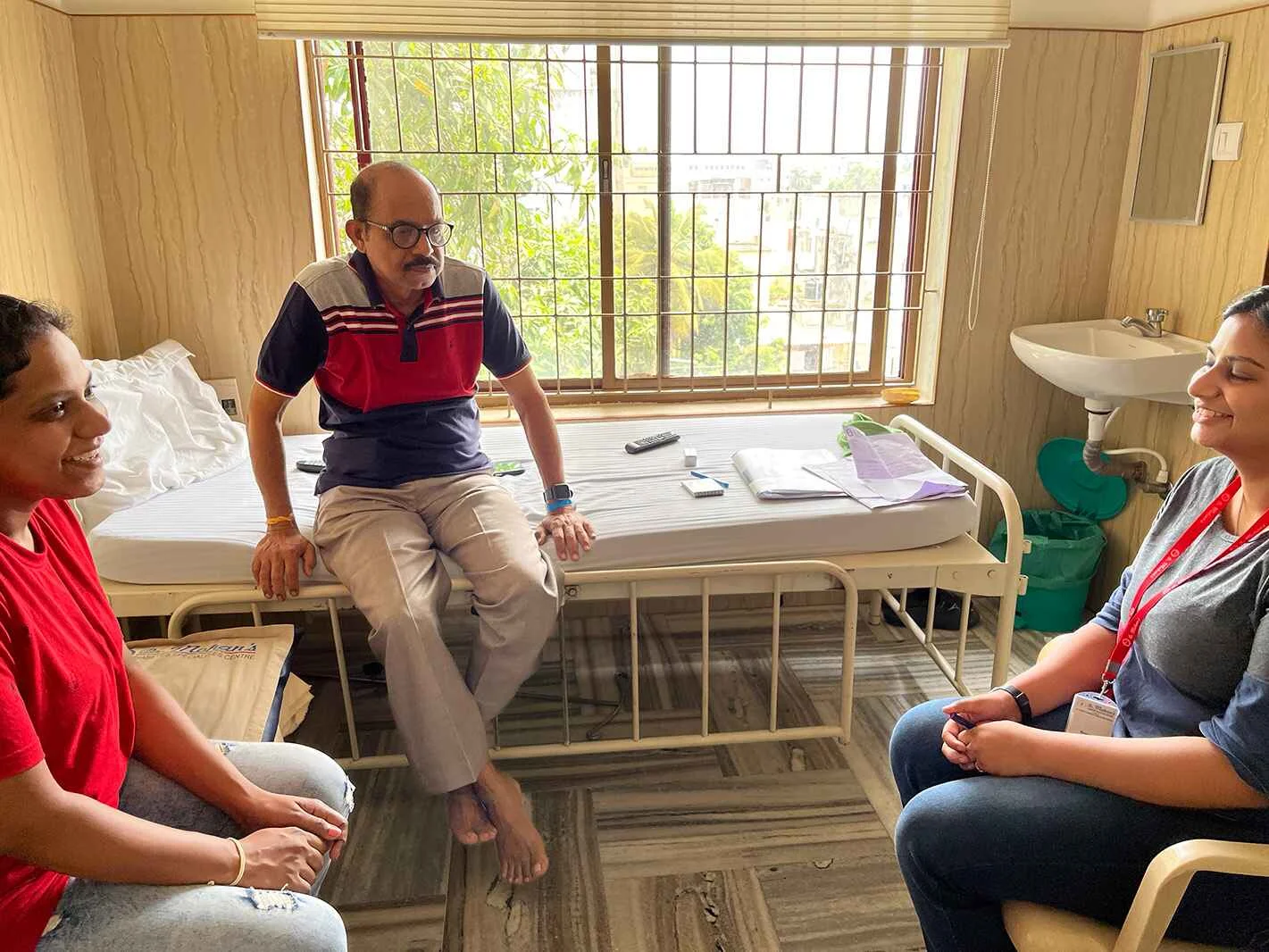
“I’ve visited many hospitals, but this is the fifth in seven years that provides good care. However, I find it challenging to come for regular check-ups because it’s far from my home.”
“After the diagnosis, I searched for guidance on what foods to include, avoid, and cooking tips by watching YouTube channels.”
“At times, the stigma of having diabetes in my early 30s feels like an extra burden. It affects not just how others perceive me but also how I perceive myself. It’s a daily battle against judgment and stereotypes.”
Insights
1. Nutrition Knowledge Gap
A significant nutrition knowledge gap among individuals with diabetes hinders informed dietary choices and optimal management.
2. Access to Trusted information
There’s a rising demand for trustable, accessible resources on diabetes prevention, management, and self-care.
3. Early Support to delay Onset
Providing early support and education can significantly contribute to delaying the onset of diabetes.
4. Systemic Challenges in Diabetes Care
The healthcare system struggles to provide comprehensive diabetes care, including coordination and addressing its multifaceted nature.
5. Constant Support and Continuous Education
Continuous support and education empower patients with the knowledge and resources for long-term diabetes management.
6. Financial Constraints
Financial barriers hinder access to essential diabetes care, medication, and healthier choices.
Persona
Developed two user personas for Type 2 diabetic patients in denial and uncertainty phases.
Ideation/ Development
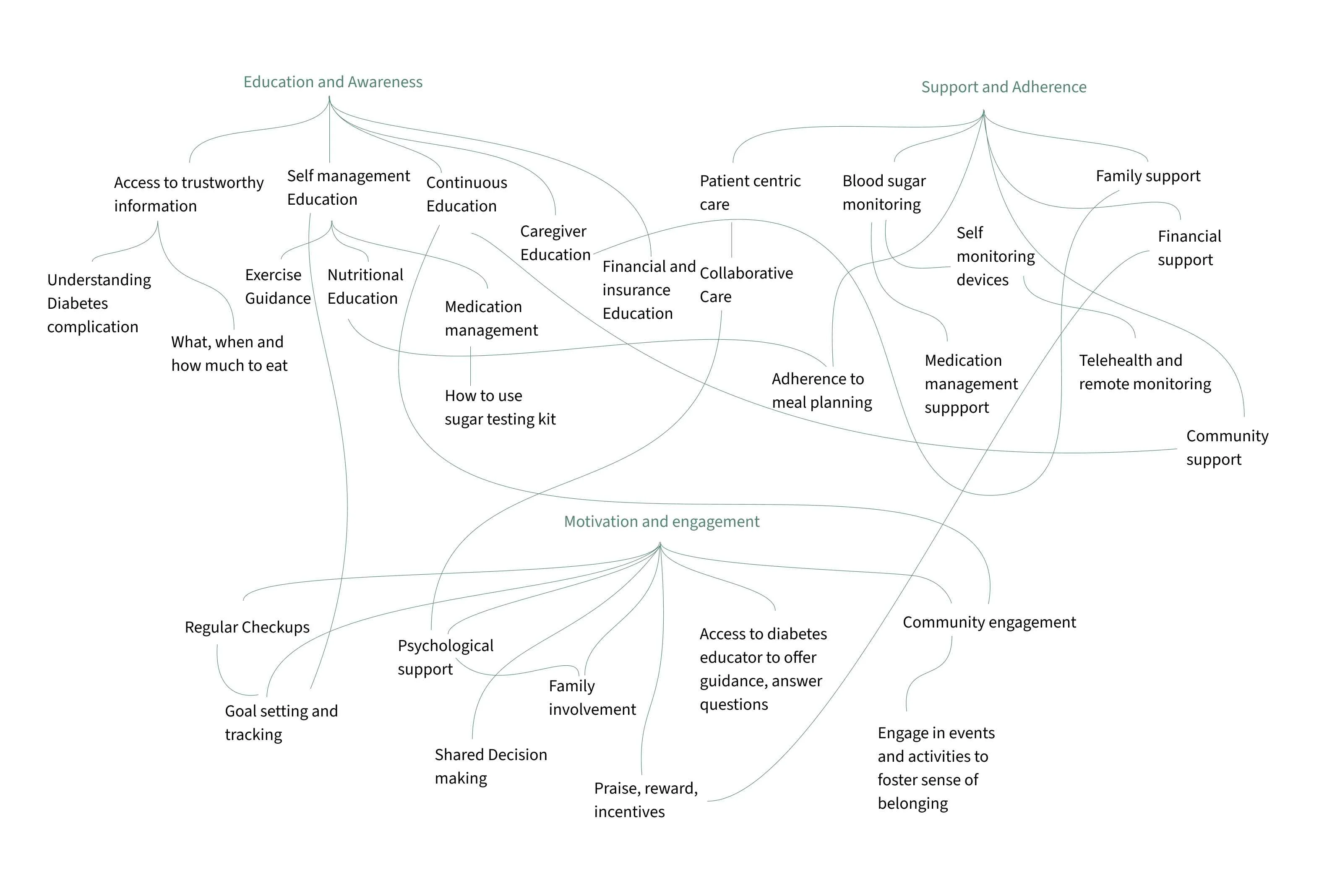
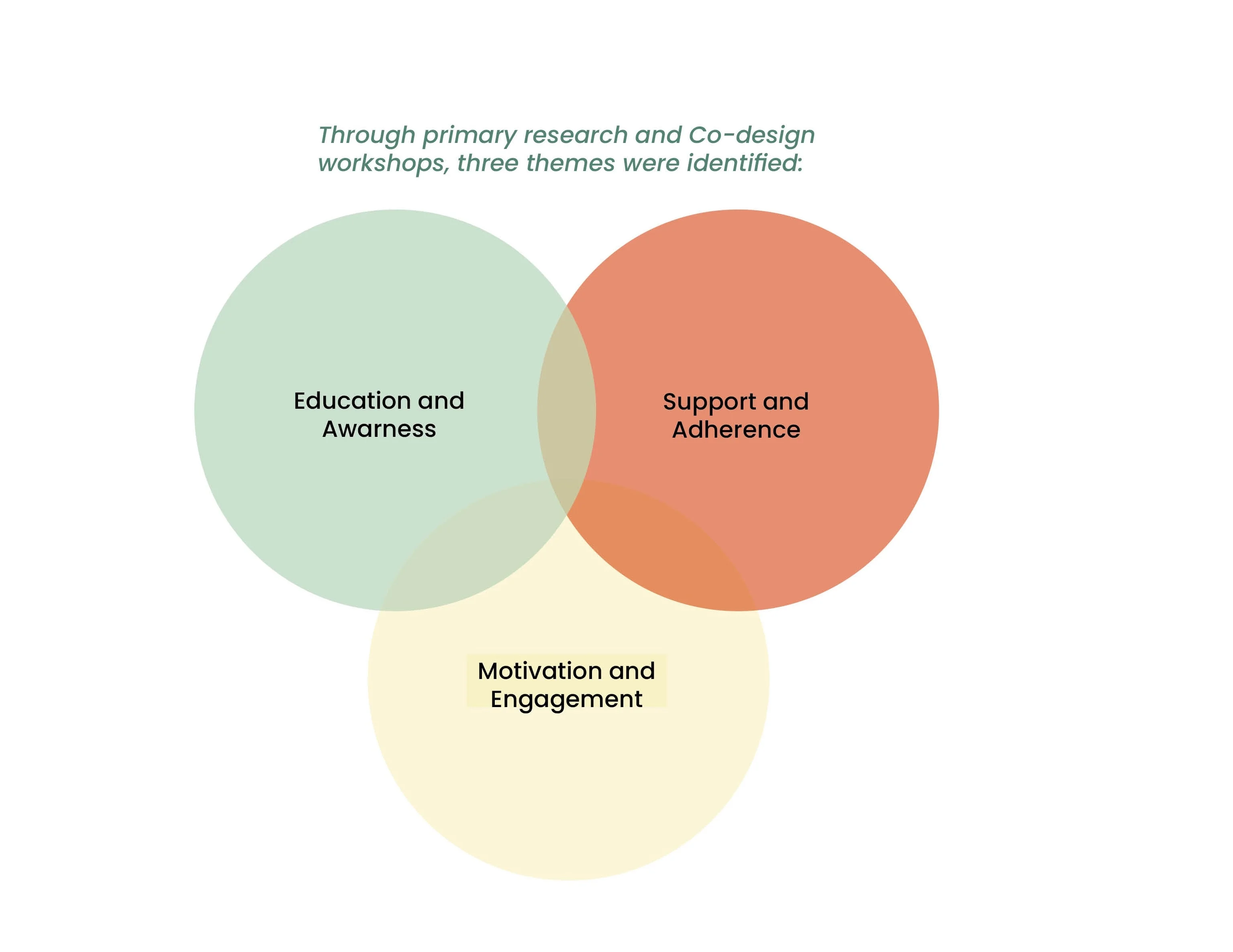
Co-Design Workshop with Diabetes Care Experts
The Co-Design Workshop was divided into three sessions and conducted with a diverse group of healthcare professionals, including diabetologists, nutritionists, psychologists, physiotherapists, and diabetes educators. The aim was to collectively identify key areas of focus within the service to enhance the early support for individuals with Type 2 Diabetes.
Part 1 - Exploring the Emotional and Practical Dimensions of Living with Type 2 Diabetes Mellitus (T2DM) from Healthcare Providers' Perspectives
Using a template, they explored the verbal expressions, thoughts, emotions, and actions of patients during periods of uncertainty and denial.

Part 2: Identifying of the primary challenge to tackle
Building on insights gathered from the empathy mapping exercise and subsequent discussions of the summarized findings, participants collectively identified the most crucial challenges to address.

Part 3: Ideation and evaluation of the chosen ideas with stakeholders.

Brainstorming and Prototype
Nirvana
A service offering support during the challenging phase of denial and uncertainty by connecting individuals with diabetes care team, providing valuable self-management resources, and facilitating access to a supportive community.

Connection with Diabetes Care Team
Users connect with a diabetes care team, comprising healthcare professionals who provide personalized support.This could involve video calls or in-person consultations, depending on user preferences and circumstances.
Self-Management Resources
Users access a variety of self-management tools/resources,to enhance their understanding of diabetes and improve self-care practices.
Community Engagement
Users are encouraged to join a supportive community where they can share experiences, ask questions, and provide support to one another. This fosters a sense of belonging and reduces feelings of isolation.
Diabetes Management Toolkit
Send periodic physical materials, such as printed guides, recipe books, or exercise charts, to complement digital resources and cater to different learning preferences.





Reflection
Challenging the traditional Model of Chronic Illness: Nirvana led me to question the conventional view of chronic illness management, where patients are seen as 'non-compliant' if they don’t follow prescribed regimens. I realized that those in the early stages of Type 2 diabetes aren't simply 'in denial'—they’re navigating complex emotional, social, and cultural factors. This shifted my focus from correcting behavior to supporting individuals in building resilience and self-agency through person-centered, compassionate strategies.
Rethinking Success Metrics in Health Design: Success in diabetes management is often measured by clinical outcomes, but this project taught me that for many, especially in early stages, success can mean accepting their condition, building confidence, or small mindset shifts. This broadened my understanding of progress, emphasizing metrics that include emotional resilience and self-awareness, not just medical outcomes.
Complexity of Behavioral Change: The complexity of behavioral change in diabetes management underscores that knowledge alone is insufficient; emotional resilience and social dynamics are equally critical in shaping individual behaviors. Emotional responses to challenges can either empower or hinder progress, while social networks provide essential support that can motivate adherence or contribute to relapse.
Embracing Uncertainty: Design as an Evolving Process: I learned to embrace uncertainty, both in the lives of those managing Type 2 diabetes and in the design process itself. I realized that as users' needs change over time—from denial to acceptance or even relapse—design solutions must adapt and evolve. This taught me the importance of flexibility, humility, and recognizing that solutions for chronic conditions are never final but must continuously grow alongside the user's journey.